Specifications:
Further Information
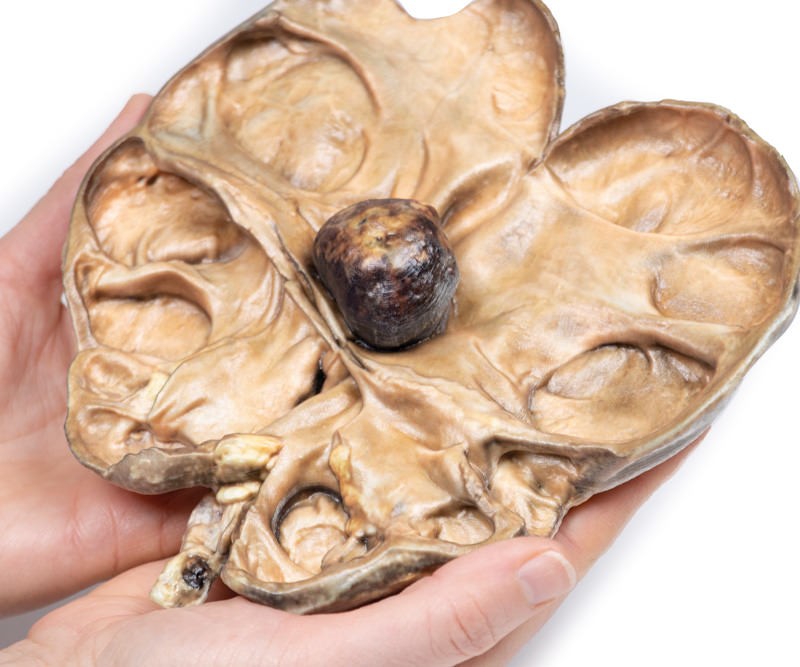
Urolithiasis (renal calculi) is a very common disease affecting up to 1 in 10 individuals during their lifetime. Formation of the stones can occur anywhere along the urinary tract but most commonly occurs within the kidneys. Risk factors for stone formation include male gender; any condition that affects the composition of the urine, such as hypercalciuria or high urine oxalate; systemic metabolic disorders, such as cystinuria and gout; dietary factors, such as high oxalate and animal protein intake, low fluid intake; and environmental factors, such as high dry temperatures. 80% of renal calculi are unilateral. Symptoms of urolithiasis include excruciating pain, haematuria, nausea, vomiting, fainting, dysuria and urgency. Symptoms depend on the size and the site of the calculus. Urolithiasis can be asymptomatic especially if the stones are formed and remain within the renal pelvis or bladder. Symptoms occur when the stones move into the ureter. Pain from calculi is usually colicky and typically severe in nature; occurring in paroxysms. The flank is the most common site for pain but pain can occur anywhere along the urinary tract and into the genitals. Pain resolves on passage of the stone. Haematuria can be gross or microscopic. Diagnosis can be made based on the medical history and examination. Radiological tools frequently used to assist diagnosis include non-contrast CT or ultrasound of the kidneys and bladder. Less commonly used imaging methods include abdominal X-ray, intravenous pyelogram and magnetic resonance imaging. If left untreated renal damage and ultimately renal failure from progressive obstruction and hydronephrosis will occur. If the obstructing calculus is not relieved it will cause pressure to build up proximal to the obstruction. This pressure is transmitted back through the collecting ducts to the cortex causing progressive atrophy of the renal parenchyma with dilatation of the renal calyces and pelvis. The pressure also compresses vasculature in the medulla leading to ischaemic medullary damage. Glomerular filtration persists in the affected kidney until late in the disease process when it will gradually diminish. Obstruction triggers an interstitial inflammatory process leading to fibrosis. Renal calculi also predispose patients to infection secondary to obstruction and the trauma that they cause to the urothelium. Treatment in acute patients include supportive treatment to allow the passage of the stone. Medical treatment used includes analgesia, commonly NSAIDs and opiates, and agents to aid passage of the stone, such as alpha blockers, calcium channel blockers and antispasmodics. Surgical intervention may be required if there are severe complications due to calculi or if the stone is large and unable to be expelled with conservative treatment. Surgical interventions include lithotripsy (using lasers or electricity), laparoscopic stone removal or percutaneous stone removal. Open surgery is rarely required.
Catalogue: PDF
See more products OpenMedis brand.









Reviews
There are no reviews yet.